To choose or not to choose? A study on decision-making for virtual reality intervention in children with ADHD
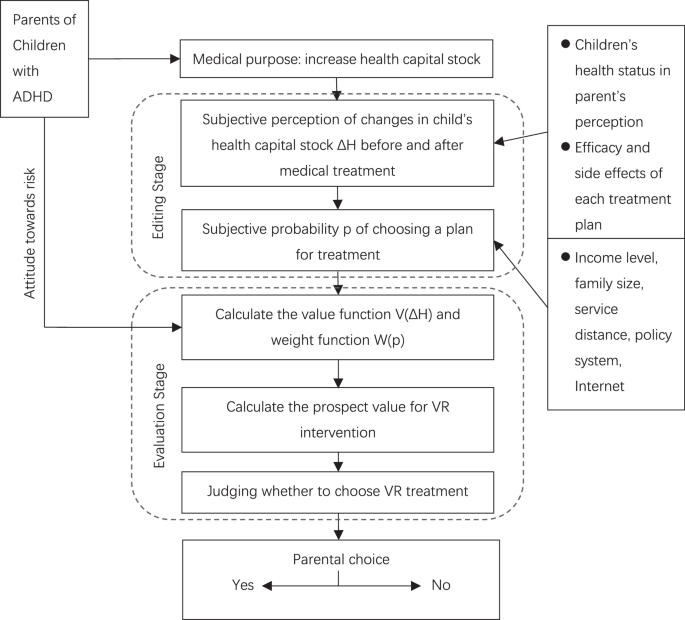
An evolving theoretical framework for behavioural decision making in healthcare choices
The behavioural decision-making in medical choices primarily investigates the decision-making process and behavioural patterns individuals exhibit when confronted with medical choices. Treatment choice is a multifaceted research subject, encompassing decisions made by individuals based on their needs, expectations, environmental resources, and external constraints (Shi 2021). In the early 1960s, scholars began to focus on medical decision-making theories (Zhang et al. 2012). Subsequent empirical studies explored the factors affecting patients’ medical behaviours, including the quality of clinical communication between parents and physicians (Salmon and Young 2013), parents’ familiarity with medical knowledge (Li et al. 2022), the content of information accessed on social media (Xu and Ma 2018; Yang and Chao 2021), the level of support provided by online communities (Sun and Kang 2022), urban-rural or cultural disparities (Brown et al. 2015; Chen et al. 2019), and household income (Abera et al. 2015), among others. These empirical investigations into patient behavioural decision-making have extended from a medical perspective to sociological, economical, psychological, and communicational domains. With the continuous evolution of research, scholars are endeavouring to devise theoretical tools that accurately depict patient decision-making(Li and Song 2010). the Andersen Model predicts medical choice outcomes from a demand and supply perspective (Andersen and Kravits 1976); the Expected Utility Theory posits that individuals’ decision-making will opt for the option with the maximum expected utility; the Mental Accounting Theory proposes that individuals categorize and evaluate economic or psychological costs and benefits in decision-making, and make decisions based on the balance of different accounts. Currently, the field of behavioural decision-making in healthcare choices faces methodological challenges, such as how to accurately collect and process data in empirical studies to measure individual preferences, emotions and cognitive processes. How to explore VR intervention choice decisions for children with ADHD based on empirical methods remains an area to be explored. This study used Prospect Theory (PT) as a theoretical framework for behavioural decision-making, which suggests that individuals’ attitudes towards risk and uncertainty in healthcare choices may not only be based on expected utility, but also be influenced by their perceptions of losses and gains. The inherent consistency of Prospect Theory with decision-making under conditions of risk makes it applicable to understanding healthcare choices.
Decision-making for VR interventions based on prospect theory
Prospect Theory, introduced by Daniel and Amos in 1979, is a behavioural economic theory designed to elucidate decision-making processes and individual characteristics under risk conditions. It posits that individuals are not entirely rational in their attitudes towards risks and rewards. Specifically, when faced with potential gains, individuals prefer certainty to risk; when faced with potential losses, people are more inclined to take a’gamble’.
In the information editing stage, parents gather information related to virtual reality from various sources; they then combine this information with their own preference structures, belief traits, and situational factors to form decisions. There are three main types of situations that influence their personal preferences: 1. Representativeness heuristic: the treatment choices and outcomes of ADHD families in the online community influence other families’ assessment of treatment options. 2. Availability heuristic: refers to the ease with which patients and their parents can access detailed information about treatments – including media reviews, advertisements released and treatment behaviours provided by physicians’ degree of guidance – the ease with which they can do so. 3. Anchoring and adjustment: a theory in psychology that measures behavioural decision-making. Factors affecting anchoring values may include the child’s condition, the parents’ mental calculations of the cost of treatment, and expectations of outcomes (Kahneman and Tversky 1979).
The time and transport costs of VRT were also key factors influencing the preference structure during the assessment phase. Parents compare the prospect of virtual reality therapy constructed in the previous phase with other methods and weigh them to make a final decision based on their mental readiness, which corresponds to the weighting function in prospect theory.
Based on the theory and logical derivation, we propose three stages of the parental decision-making process. In the first stage, by compiling information about the treatment plan to form a belief profile, parents determine the expected value of their child’s health stock based on their own beliefs and preference structure; by ‘simplifying and synthesising’ the expected value and its influencing factors, they are prepared for subsequent risk assessment and decision-making choices. In the second stage, the patient’s preference structure is assessed, the parents calculate the expected value of the virtual reality (VR) intervention technology, and the information collected in the editing stage is measured to generate a value function and a weighting function. The third stage is then the patient’s healthcare behavioural decision, where the parents decide whether to choose the virtual reality intervention technology for their child (Fig. 1).
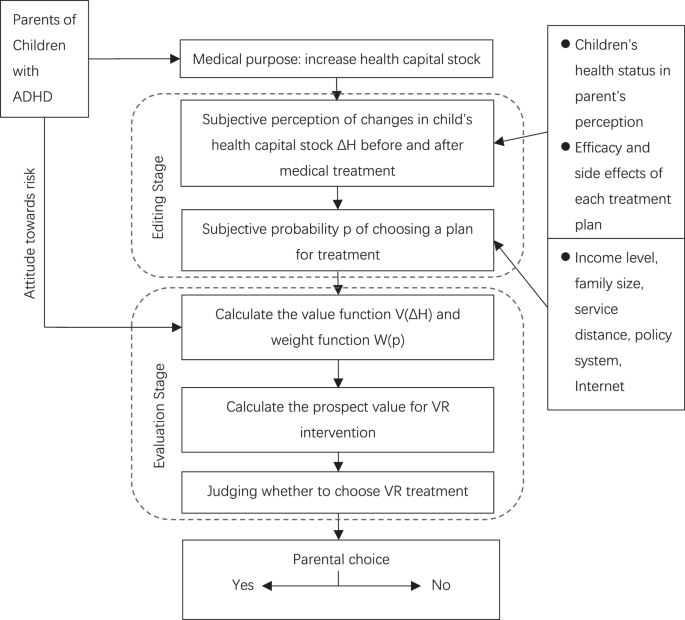
Including two stages, upper dotted box shows the editing stage, where different “prospects” (child’s health capital stock, effects of each treatment, etc.) are simplified and recoded. Lower dotted box shows the evaluation phase, where the edited prospects are evaluated and the highest-value choice is ultimately made.
The use of virtual reality in the treatment of ADHD in children
Studies have shown that medication, the first treatment option considered, is not ideal in practice due to children’s family and personal factors, such as on-time and adherence to medication (Wang et al. 2020). At the same time the focus on children with ADHD in the fields of behavioural, neuroimaging and genetic sciences has provided new perspectives and stimulated new therapeutic approaches to our understanding of the underlying pathophysiological mechanisms of ADHD (Shaw et al. 2014). Virtual reality intervention techniques, as an emerging therapeutic approach, offer some advantages over traditional pharmacological treatments (Bashiri et al. 2017).
Virtual Reality (VR) technology replaces user perception in the real world by digitally generating perceptual experiences. It has the advantages of being immersive, easy to operate, not limited by time and space, and accurately simulating real-world scenarios. In the field of behavioural interventions, VR technology has been combined with classroom tasks (Bioulac et al. 2020), serious games (Rodrigo-Yanguas et al. 2021), physical training (Shema-Shiratzky et al. 2019), and neurobiofeedback training (Oh et al. 2022), proving its effectiveness in reducing the attention shifting frequency and enhance patients’ cognitive abilities and executive function.
By creating a precisely controlled virtual world for the user, virtual reality technology facilitates therapeutic interventions (Freeman et al. 2017; Hatta et al. 2022b, 2022a). Numerous studies have confirmed the ability of VR technology to create virtual environments for diagnosis, training, monitoring, assessment and treatment to provide optimal rehabilitation for children with ADHD (Bashiri et al. 2017; Romero-Ayuso et al. 2021). Studies have identified key advantages of virtual reality as a treatment modality for ADHD: (1) providing a safe and controlled environment for children to practice and develop cognitive skills such as attention and impulse control; (2) enabling children to manage distractions and improve attention by immersing them in a virtual environment; (3) providing a non-pharmacological alternative for children with ADHD who are intolerant or unresponsive to medication; (4) serve as a valid assessment tool to better evaluate ADHD symptoms and improve diagnostic accuracy; and (5) demonstrate effective outcomes in terms of enhanced sustained attention, measures of alertness, increased number of correct responses, and reduced number of errors of omission (Schweitzer and Rizzo 2022). Despite the encouraging short-term results of VR interventions for ADHD, the effectiveness, feasibility, and adaptability of VR as a treatment modality need to be validated through long-term research data. Currently, there is a lack of clinical trial data to support its long-term effects and potential side effects; the requirement for specialised equipment and technical support results in high costs; and some children have shown adverse reactions to VR technology, experiencing symptoms such as dizziness and headaches during assessment or training.
In summary, this study identifies the factors that influence parents’ willingness to choose a virtual reality intervention programme for their children based on a prospective theoretical framework and classifies them into three categories: 1. Preference structure, which includes the price and time costs parents are willing to pay, and demographic and individual characteristics of parents; 2. Belief characteristics, encompassing media reviews, advertisement releases, the extent of treatment behaviour guidance provided by doctors, the child’s condition, parents’ psychological calculations of treatment costs, and their expectations of treatment outcomes; 3. Online community involvement, referring to the information parents acquire through participation in online communities.
Based on the above, we propose the following hypotheses:
H1: Preference structure influences parents’ decision readiness.
H2: Belief characteristics influence parents’ decision readiness.
H3: Online community involvement affects parents’ decision readiness.
H4: Parents’ decision readiness ultimately leads to their decision.
Using the research hypotheses and variable settings, we establish a structural equation model to describe the decision-making path and outcomes of patient medical behaviour. The model comprises four latent variables: belief characteristics, preference structure, community involvement, and decision readiness. From a relationship perspective, belief characteristics, preference structure, and community involvement influence decision readiness, which in turn affects the final decision outcome (Fig. 2).
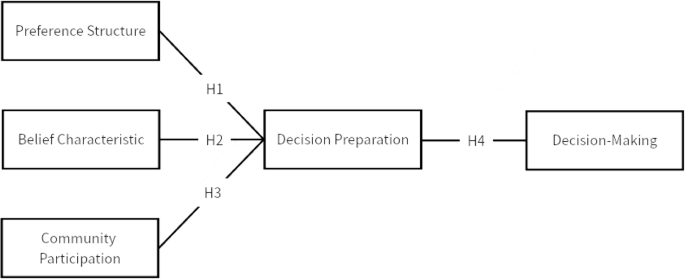
A structural equation model includes variables of belief characteristics, preference structure, community involvement that influence decision preparation, ultimately affect decision making.
link





