Comprehensive evaluation of medical quality and analysis of obstacle factors in specialized neurological hospitals based on a multi-dimensional evaluation model: a case study of China’s National Regional Medical Center for Neurological Diseases
This study conducted scientific analysis of selected indicators and data from the “National Evaluation” during 2019–2023, revealing progressive enhancement in comprehensive medical quality at this tertiary specialized neurological hospital. Obstacle degree analysis further indicated significant improvement in medical service volume, despite persistent medical safety challenges requiring targeted interventions. Additionally, social evaluation and operational efficiency metrics warrant management attention.
Progressive improvement in comprehensive medical quality
The integrated approach combining entropy-weighted TOPSIS and RSR methods—both widely applied in health management—demonstrated high consistency between their evaluation results. This methodological convergence not only validates the reliability of findings but confirms substantial improvement in the hospital’s comprehensive quality. Since implementing the National Performance Evaluation for Tertiary Public Hospitals in 2019, continuous medical quality optimization has been observed, evidencing the comprehensiveness and scientific validity of the evaluation framework. This system enables objective assessment of hospital operations and service quality, facilitates precise identification of management weaknesses, and supports targeted process optimization—providing critical guidance for high-quality development. Notably, the significant decline in performance during 2020 (ranked 5th by both TOPSIS and RSR methods) coincides with the peak of the COVID-19 pandemic in China. The containment measures implemented that year—including lockdowns, suspension of non-urgent services, and resource diversion—may account for this anomaly.
Analysis of key influencing factors
Entropy-weighted TOPSIS results indicated that social evaluation indicators collectively carried the highest weight (22.94%), consistent with obstacle degree analysis showing three social metrics (outpatient/inpatient/staff satisfaction) ranking within the top five barriers during four of the five years. This pattern indicates a significant potential for improvement in social evaluation. Medical service volume (21.54% weight) demonstrated decreasing obstacle degrees annually, likely contributing to overall quality enhancement. Service efficiency (19.58% weight) showed significantly increased obstacles in 2020 before stabilizing, warranting management intervention. Operational efficiency (19.44% weight) displayed progressively increasing obstacle degrees requiring attention. Despite the indicator for low-risk mortality (X10) having the highest individual weight (11.40%), the Medical Safety dimension received the lowest overall weight (16.49%). This paradox stems from the mathematical principle of the entropy weight method—weight assignment prioritizes data variability over clinical significance: It objectively quantifies data dispersion but fails to capture managerial criticality. In this study, the obstacle degree model effectively bridged this gap: medical safety indicators were persistently identified as core obstacles because their actual performance deviated from ideal values (e.g., X10 reached a negative peak of 1.010 in 2021). Consequently, healthcare quality evaluation must integrate objective weighting (entropy method) with managerial prioritization (obstacle model)—the former reduces subjective bias in weight allocation, while the latter reveals improvement urgency by diagnosing deviations from optimal performance. This dual approach is particularly critical for specialty hospitals, where clinical safety risks inherently demand prioritized intervention.
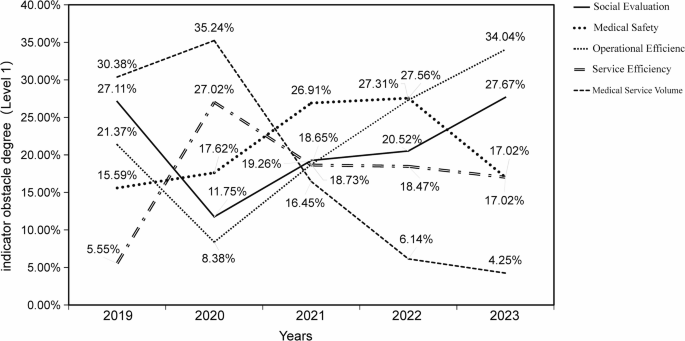
It is noteworthy that a sharp reduction in outpatient visits (X1 = 0.010), surgical procedures (X2 = 0.010), and hospital discharges (X3 = 0.010) in 2020 was directly linked to the suspension of elective surgeries and routine outpatient services during the pandemic. This explains the transient contraction in service volume, which rebounded rapidly after 2021.Infection control protocols prolonged disinfection intervals, resulting in the lowest bed turnover rate (X5 = 0.010) and bed occupancy rate (X4 = 0.010) in 2020. Concurrently, the average length of stay (X6 ranked 2nd worst) increased due to a higher proportion of complex cases and strained rehabilitation resources. Cost indicators such as per-visit outpatient expenses (X7 = 0.520 vs. 0.010 in 2019) surged significantly, primarily driven by PPE expenditures.Patient satisfaction scores (X12 = 0.010; X13 = 1.010 inverted ranking) declined due to visitation restrictions and service delays. In contrast, staff satisfaction (X14 = 1.010 inverted ranking) temporarily rose, attributable to crisis-driven solidarity. These fluctuations stabilized as pandemic pressures eased. Low-risk mortality rates (X10 = 0.010) remained stable, indicating unimpaired core safety protocols; however, the increase in complication rates (X11 = 1.010) may reflect delayed presentations of severe cases, warranting ongoing vigilance. Obstacle degree analysis (Fig. 1) revealed a sudden spike in operational efficiency barriers (e.g., cost metrics X7–X9) in 2020, aligning with pandemic-induced transient cost increases. By contrast, medical safety barriers showed no significant deterioration, underscoring institutional resilience during the crisis. The temporal overlap between the 2020 peak in operational efficiency obstacles (~ 30%) and the pandemic period—while medical safety barriers remained stable—further substantiates the temporary nature of these external factors.
Targeted recommendations for sustainable quality improvement
Enhancing social evaluation
Improve staff satisfaction by implementing merit-based compensation systems that recognize technical expertise, supporting healthcare workers in developing core competencies22. For patient satisfaction, address non-medical service needs through improved clinician-patient communication, optimized appointment scheduling (e.g., segmented visits, digital solutions), and regulation of clinical behaviors using DRG/clinical pathways to reduce excessive prescriptions and enhance trust23,24.
Optimizing service efficiency
For service efficiency enhancement: Expedite medical consortium collaboration to implement primary care prioritization and two-way referrals, rationally allocate medical resources. Promote clinical pathways to shorten average length of stay (ALOS), accelerate bed turnover, and improve overall bed utilization. Adopt hospital-wide unified bed management by establishing pre-admission service workflows that relocate preoperative assessments before hospitalization, reducing ALOS while enhancing patient satisfaction25. Implement additional ALOS-reduction strategies including day/micro-surgeries, clinical pathway optimization, and multidisciplinary diagnosis-treatment pathways26.
Regarding medical expense management: Pharmacists should strengthen clinical support to assist physicians in rational medication use—The identification of Drug Expenditure Ratio (X9) as a top-five obstacle in 2023 (Obstacle degree: 17.02%) necessitates targeted interventions for medication cost control. By integrating administrative interventions, pharmaceutical expertise, and evidence-based prescribing practices through departmental collaboration, the drug expenditure ratio can be effectively reduced. We therefore recommend establishing a real-time prescribing feedback system embedded in EHR, which alerts physicians when high-cost alternatives exceed therapeutic benefit thresholds, reduce unnecessary costs, and continuously optimize prescription structures27. This directly addresses X9’s core obstacle mechanism – unoptimized medication selection patterns. Concurrently, conduct timely analysis of operational cost structures to establish targeted incentive mechanisms ensuring reasonable cost allocation—reducing expenditures on pharmaceuticals, consumables, and diagnostic tests28. Under the guiding principle of “aggregate control, structural adjustment, selective increases/decreases, and phased implementation”, reinforce cost controls by decreasing drug/consumable expenses29. In addtion, the identification of Cost per Hospitalization (X8) as the top obstacle in 2023 (Obstacle degree: 17.02%) reflects persistent cost-control failures in high-risk surgical procedures, we therefore propose implementing a real-time consumables PDCA cycle comprising: Alerting for consumables exceeding preset thresholds by > 15% to incentivize cost-conscious practices.
Integrated medical safety strategy for neurological hospitals
Given the specialty’s inherent characteristics—including anatomical complexity, high-risk complication propensity, technically demanding procedures, significant individual variations, and intricate perioperative management—medical safety remains a persistent critical barrier. Therefore, medical safety constitutes the paramount priority in hospital administration. Key measures include: we will focus on three critical indicators—complication rate (X11), low-risk mortality rate (X10), and surgical volume (X2)—requiring urgent systemic reforms to overcome management bottlenecks and achieve dual improvements in healthcare quality and safety efficacy. First, reducing Complication Rate (X11), a perioperative full-chain risk prevention and control system should be established, implementing closed-loop management spanning preoperative-intraoperative-postoperativephases. Artificial intelligence (AI)-powered neuro-navigation robotic-assisted surgery should be leveraged to minimize intraoperative nerve injury risks. Second, controlling Low-Risk Mortality Rate (X10), a dual closed-loop system integrating regional emergency coordinationand quality controlmust be developed. Leveraging the medical consortium framework, a green transfer channelfrom primary hospitals to regional centers should be established, supported by 5G-enabled teleconsultation systems and dedicated ambulances to ensure optimal treatment timelines. Additionally, a standardized regional emergency training curriculum should be implemented, mandating uniform competency development for all primary care medical staff to ensure homogeneous skill proficiency. Third, ensuring Surgical Volume (X2), an innovative resource allocation and efficiency enhancement model is needed, including a cross-institutional surgical scheduling system that dynamically integrates underutilized regional operating room capacity to maximize patient safety and procedural throughput. In addition, implementing evidence-based intervals between consecutive surgeries (excessive intervals waste resources while insufficient intervals compromise sterilization, causing iatrogenic infections30; establishing real-time surveillance of surgical complications, particularly in high-risk departments, to identify causes and contain risk factors; reducing hospital-acquired infection-related complications and low-risk mortality; conducting root-cause analysis of adverse surgical outcomes to identify vulnerabilities; and organizing specialized case reviews for departments with elevated complication rates to enhance safety awareness, document lessons learned, and prevent recurrence.
Limitations
The social evaluation indicators in this study, collected through hospital self-reporting systems, may be subject to response bias (patients potentially inflating satisfaction ratings due to doctor-patient relationship concerns, especially in face-to-face surveys) and sampling bias (lower response rates through third-party platforms designed to avoid face-to-face bias), which could affect the social evaluation dimension’s obstacle degree analysis results. While the single-site evaluation at Tianjin Huanhu Hospital – the regional medical center for neurological disorders in North China – enhances internal validity, its scale and regional centrality constrain generalizability to smaller or contextually distinct neurological hospitals. This limitation is compounded by the study’s reliance on the National Performance Evaluation Guidelines for Tertiary Public Hospitals, a generalized framework lacking integration of critical neurological-specific metrics. Consequently, findings may inadequately reflect specialty-unique performance dimensions and hinder broader applicability. Future work should be considered from the following two aspects: Given China’s vast territory, we will establish additional sub-centers in healthcare institutions across Eastern, Western, and Southern regions. Selection criteria will prioritize institutions with diverse geographic distributions and high annual patient volumes. This expansion aims to improve the study’s breadth through rigorous external validation. Additionally, we will explore specific neurological outcome measures, such as the Modified Rankin Scale scores or postoperative functional indices (e.g., neurophysiological recovery trajectories). These granular assessments will improve the study’s robustness.
link







